What do HPV completion rates say about women’s access to health care?
By Gwen Emmons
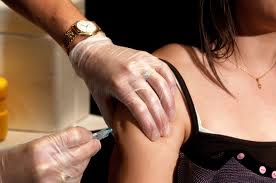 After a difficult fight to approve the HPV vaccine (and defend it from opponents who claimed the vaccine causes promiscuity, “mental retardation,” and a host of other head-scratching claims), the news that less than one in four women actually complete the vaccination series is alarming.
After a difficult fight to approve the HPV vaccine (and defend it from opponents who claimed the vaccine causes promiscuity, “mental retardation,” and a host of other head-scratching claims), the news that less than one in four women actually complete the vaccination series is alarming.
The study, conducted by researchers at the University of Texas, showed that completion rates of the three-part vaccine plummeted between 2006 and 2009. The sharpest decline was among women ages 9 to 18 – precisely the age group that benefits most from the vaccine since they are less likely to have contracted HPV.
The precipitous decline is frustrating, but it also highlights the gaps women – especially young women, poor women, and women of color – face in accessing health care on a daily basis. As women are missing appointments for follow-up shots, what else are they missing out on – and why?
The UT study offers a few clues. For starters, study authors found that areas with higher concentrations of pediatricians were more likely to be up-to-date on all their vaccines. More doctors in a community often means shorter wait times and the luxury of choosing a provider a patient can trust – both factors that can encourage the maintenance of a strong health care routine. However, lower income communities often lack an adequate network of health care providers. Longer waits for appointments, more distant travels to doctors’ offices, or even just not knowing how to find a doctor can stand in the way of getting all three required shots of the HPV vaccine – but such barriers can also limit access to regular well-woman visits, preventative service appointments, and prenatal care.
Poor HPV completion rates make a case for making long-term relationships between a woman and her medical provider a priority. Those who started the vaccination series with an obstetrician or gynecologist were more likely to complete the series than those who started with a pediatrician, possibly due to a gap that often exists between a woman’s pediatric care and her gynecological care. Therefore, if a woman starts the HPV series with her pediatrician, but fails to transition into the care of a trusted gynecologist or other primary care provider, obtaining the final one or two vaccinations can be impossible. It also means women may skip STI screenings, pap smears, and other services vital to women in their late teens and early twenties. As women age, pediatricians would be wise to start a dialogue with their patients about the next step of care – and help their patients find a new provider. Adolescent medicine could play a unique role in transitioning teens from a pediatrician to a gynecologist or adult care provider, while remaining attuned to the unique needs and concerns of adolescents.
Poor completion rates may also be due to a perceived inability to access the vaccine without parental knowledge. A 1998 survey showed that only 8.4% of adolescents have accessed healthcare services confidentially; less than half even knew where to go to access confidential care. Since visits to a pediatrician are almost always with a parent in tow, adolescents may feel uneasy about requesting the vaccine or less empowered to follow up on the rest of the vaccination series. Yet again, adolescent medical providers attuned to teens’ privacy concerns could enhance compliance – but medical providers of all specialties would be wise to recognize the unique concerns of adolescents and tailor their medical interventions appropriately.
But many women turn to community health centers or emergency rooms for care, creating a host of other challenges in obtaining all three HPV shots, according to the study. Women who received their first vaccine from a “clinic, hospital, or other facility” were less likely to complete the full vaccination series, a point the authors attribute in part to the difficulty in seeking “continuous care” in clinic settings. Yet with the impending rise in community health care clinics thanks to the Affordable Care Act, community health care providers should identify potential gaps in services and work with patients to create a plan of care, such as walking them through how to schedule a follow-up appointment, brainstorming with them how to juggle work and family obligations so they can attend appointments, and informing them of the importance of follow-up care. The authors posit that text message reminders about follow-up visits might improve compliance. The potential for a woman to change her cell phone number (or not have a cell phone at all) – rendering her unreachable – makes this an imperfect solution, but one that could still help thousands remember their appointments. It’s already being used to deliver valuable pre- and post-natal health information to pregnant women.
Co-pays for the vaccination series may stand in the way of women getting all three shots, especially when coupled with fees for physician visits, transportation, child care, and missed work (for the patient and/or her parents). Programs like Vaccines for Children, which provides no-cost vaccines to “Medicaid-eligible, American Indian, or Alaska Native” children, children without insurance,” and children whose insurance doesn’t cover vaccination – may be the reason why women with public insurance were more likely to complete the HPV series than women with private insurance. Let’s just hope that these programs survive rounds of budget hacks in the name of “fiscal restraint.”
Finally, thinking more critically about how we market vaccines that require multiple steps is important, especially for women who don’t regularly visit their health care provider for the reasons stated above. Gardasil was released to the public in a parade of slick commercials and magazine advertisements – but as Amanda Marcotte points out, those advertisements downplayed (or outright ignored) the vaccine’s three-step process. “I wanna be one less (after three shots)” isn’t quite as catchy, but women may not be “one less” if they don’t complete the full series. You tell me which is more important.
The failures in getting more women to complete the vaccination series speak to broader public health concerns, particularly for women who are already disadvantaged in the health care system. Receiving a vaccination series or a Pap smear often requires taking time off work, scheduling childcare, finding transportation, and having sufficient insurance (to say nothing of knowing they need care and where to find it). Each of these steps can prove to be a barrier in accessing the health care services a woman seeks. Heeding the findings of the UT study isn’t just important for vaccination compliance – it’s crucial if we’re to break down the structural barriers in our health care system that routinely deny women access to the care they deserve.
____________________________________
 Gwen Emmons is a writer and activist currently pursuing her MSW in Philadelphia. You can read more of Gwen’s work at www.GwenEmmons.com.
Gwen Emmons is a writer and activist currently pursuing her MSW in Philadelphia. You can read more of Gwen’s work at www.GwenEmmons.com.




4 Comments